| View printer-friendly version |
| Back |
|
Gap Separates Payers and Physicians on Value-Based Arrangements, According to a New Study Released by FTI Consulting
|
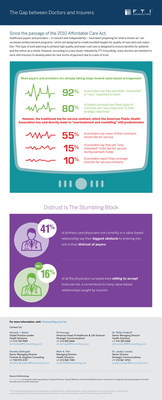
According to the study, 41 percent of primary care physicians, who are not currently in a value-based relationship, say their biggest obstacle before agreeing to enter into one is their distrust of payers. The study also found that only 16 percent of all physicians surveyed were willing to accept the financial risk – a key element of many value-based relationships sought by insurers.
"As today's healthcare environment continues to evolve, both payers and providers will need to cooperate to address the critical challenges facing the industry," said
"This lack of trust will be a huge hurdle for payers to overcome as they often cite provider buy-in and engagement as critical to the success of any value-based arrangement," said Dr.
Since the 2010 Affordable Care Act ("ACA"), healthcare payers and providers, both in concert and independently, have been preparing for value-based reimbursement programs in which meeting quality-of-care and cost-reduction targets would result in benefits for both groups and the nation as a whole. This has manifested itself in the growth of Accountable Care Organizations ("ACOs"), bundled arrangements and new relationships that have blurred the lines between insurers and providers.
In bundled payments and other value-based arrangements, many experts believe it is essential that payers and providers eventually share risks to control costs and improve quality. However, the study found that the gap between them continues to widen. Payers believe that a mere five percent of providers are willing to accept the downside risks necessary for value-based arrangements to work.
Risk-sharing is not the only perceptual disconnect between payers and providers. Payers seeking to partner with providers in value-based arrangements have identified capabilities they wish potential partners would possess. Payers want to see providers invest in Healthcare IT ("HIT"), especially in software and systems supporting clinical integration and Population Health Management ("PHM"). Eighty percent of payers say they would be likely to contract with a clinically-integrated hospital and provider system. However, only 50 percent of healthcare providers report that their organizations have implemented new technology or software to support PHM and value-based reimbursement, 32 percent have not, and 18 percent either "don't know" or are "unsure".
Most payers and providers are taking steps to prepare for the value-based arrangements incentivized by the ACA. Eighty percent of payers in the survey say these types of contracts are "very important" to their strategic objectives, and 92 percent of providers say they are either "somewhat" or "very important" to them. However, the traditional fee-for-service contract still predominates in the healthcare industry. Fifty-five percent of payers say that many of their commercial contracts remain fee-for-service, and only 10 percent report that they no longer have any fee-for-service contracts. At the same time, 15 percent of polled providers say they are "only interested" in the fee-for-service reimbursement model, which the
"Despite their disagreements, payers and providers overwhelmingly recognize the importance of value-based arrangements to promote their broader strategic objectives," said
The full survey findings from
Methodology
About
+1.202.312.9100
Investor Contact:
+1.617.747.1791
mollie.hawkes@fticonsulting.com
Media Contact:
+1.212.850.5726
peter.kerr@fticonsulting.com
Photo - http://photos.prnewswire.com/prnh/20140729/130929
SOURCE